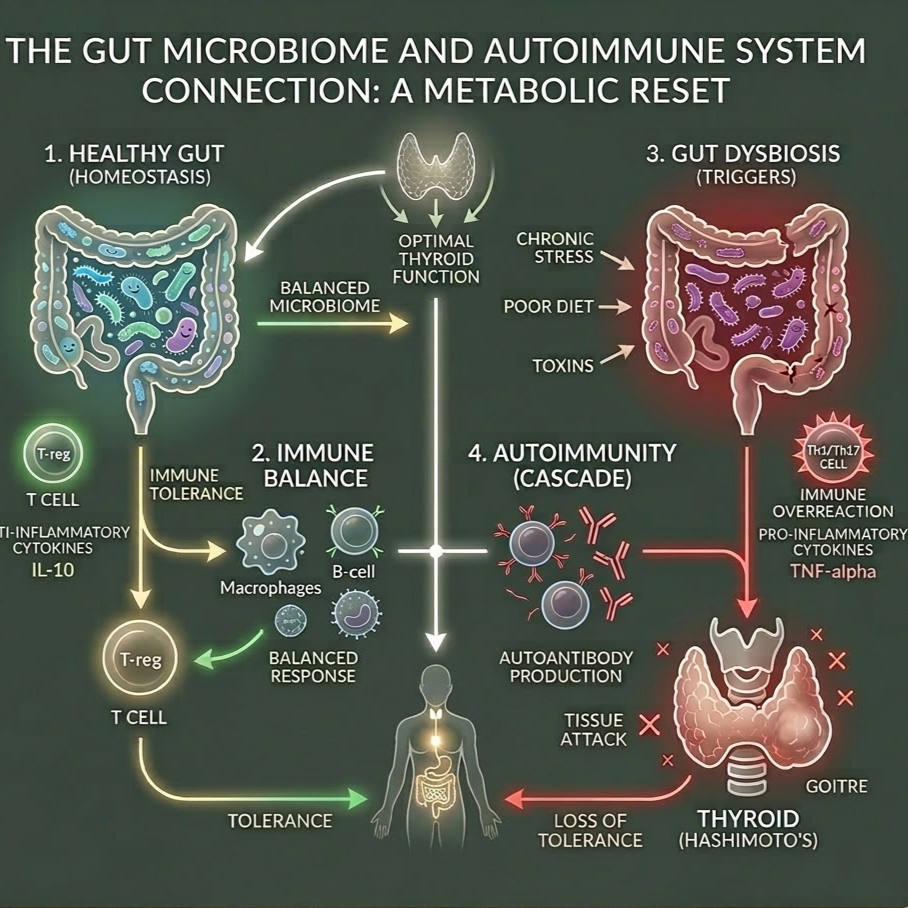
Immune System Health: Connecting the Human Microbiome to Autoimmune Disorders
The human body is home to trillions of microbes-bacteria, viruses, and fungi that live on the skin, in the mouth, and throughout the digestive tract.
Together, these microorganisms form what scientists call the human microbiome.
For many years, microbes were mainly associated with infection and disease. Today, science is revealing something very different: these microbial communities play a fundamental role in regulating the immune system.
In fact, the relationship works both ways — the immune system shapes the microbiome, and the microbiome helps train and regulate the immune system.
When this relationship is healthy and balanced, the immune system functions effectively. But when the microbial ecosystem becomes disrupted, the consequences may include chronic inflammation and autoimmune disease.
The Gut–Immune System Connection
Around 70–80% of the immune system is located in the gut.
This makes the digestive tract the body's largest immune training centre.
Beneficial gut bacteria help the immune system:
Recognise harmful pathogens
Avoid attacking harmless substances
Maintain a balanced inflammatory response
Protect the integrity of the intestinal lining
When the microbiome is diverse and stable, the immune system tends to remain calm and regulated. However, when this microbial balance is disrupted, a state known as dysbiosis, immune signalling can become dysregulated.
Dysbiosis and Autoimmune Disease
“Dysbiosis” refers to an imbalance in the microbial community, where beneficial bacteria decline, and potentially harmful microbes become more dominant.
This imbalance can occur for many reasons, including:
Repeated antibiotic exposure
Highly processed diets
Chronic stress
Environmental toxins
Poor sleep and lifestyle factors
When dysbiosis occurs, the gut barrier may become more permeable. This allows fragments of bacteria, toxins, and partially digested food particles to enter the bloodstream.
The immune system may then respond with increased inflammation and immune activation.
In genetically susceptible individuals, this process may contribute to autoimmune diseases such as:
Hashimoto’s thyroiditis
Rheumatoid arthritis
Multiple sclerosis
Psoriasis
Inflammatory bowel disease
Type 1 diabetes
Another proposed mechanism is molecular mimicry, where microbial proteins resemble human tissues closely enough to confuse the immune system and trigger autoimmune reactions.
Microbes Beyond the Gut
While the gut microbiome receives most attention, scientists are discovering that other microbial communities in the body may also influence immune health.
The oral microbiome, for example, has been studied for its potential role in autoimmune disease through processes such as microbial translocation and immune activation. Recent research is also exploring how skin microbiota may influence autoimmune conditions.
Early studies have suggested links between skin microbes and diseases such as systemic lupus erythematosus, while microbial communities in the mouth and nasal cavity may influence the progression of multiple sclerosis.
These discoveries highlight how the body’s microbial ecosystems are interconnected with the immune system in ways we are only beginning to understand.
Supporting the Gut to Support the Immune System
Autoimmune diseases are complex and influenced by many factors, including genetics, environment, and lifestyle.
However, one area gaining increasing attention is the possibility that restoring microbial balance may help regulate immune function.
Supporting the microbiome may involve several key strategies:
Eating Microbiome-Friendly Foods
A diverse diet rich in fibre and plant nutrients helps feed beneficial bacteria.
Examples include:
Vegetables and leafy greens
Garlic and onions
Berries and colourful fruits
Fermented foods such as kefir, yoghurt, and sauerkraut
Reducing Ultra-Processed Foods
Highly processed foods, excess sugar, and artificial additives may negatively affect microbial diversity and promote inflammation.
Supporting the Gut Lining
Nutrients such as glutamine, zinc, and omega-3 fatty acids may help support intestinal barrier function.
Addressing Lifestyle Factors
Sleep, exercise, and stress management all influence both the microbiome and the immune system.
A New Perspective on Immune Health
For decades, autoimmune diseases have largely been treated by suppressing immune activity.
While these treatments can be important, research into the microbiome is opening a new perspective, one that focuses on restoring immune balance rather than simply suppressing immune function. The health of the immune system cannot be separated from the health of the microbiome. Supporting the gut ecosystem may therefore become one of the most important foundations of long-term immune health.
At Lantern Clinic
At Lantern Clinic, we take a root-cause approach to chronic health conditions.
When patients present with inflammatory symptoms, fatigue, digestive problems, or autoimmune conditions, we often explore the health of the gut microbiome as part of a broader functional medicine assessment.
By addressing microbial balance, gut barrier health, and lifestyle drivers of inflammation, our goal is to help patients move toward greater resilience, better immune regulation, and long-term health.
Discover Your Gut Health Pattern
Many people experience symptoms of gut imbalance without recognising the underlying cause.
To help you understand your digestive health better, we have created a Gut Health Quiz that highlights patterns commonly associated with dysbiosis, food sensitivities and digestive imbalance.
Taking the quiz takes just a few minutes and can provide helpful insight into whether your gut may benefit from further investigation or support.