The Truth About Gut Microbiome Testing in the UK
A doctor’s guide to what works, what doesn’t and when it actually matters
Over the past few years, gut health has become one of the most talked-about topics in medicine. Patients come to us every week asking:
“Should I do a gut test?”
“Which one is the best?”
“Will this explain my symptoms?”
And the honest answer is:
👉 Gut microbiome testing can be powerful, but only when used correctly.
As a UK-trained GP with vast NHS experience and advanced training in functional medicine, I’ve seen both sides:
The limitations of conventional testing,
And the potential of a deeper, root-cause investigation that brings valuable information and clarity.
This guide will give you a clear, evidence-informed, clinically grounded understanding of:
What gut tests actually measure?
Which ones are worth considering?
Their limitations (often overlooked)
And whether they are right for you
What is a gut microbiome test really?
A gut microbiome test analyses a stool sample ( 1-3 days of stool samples)
Bacteria
Fungi
Parasites
Digestive function: how is the food digested and absorbed
Inflammation and immune activity at the gut lining level.
This is fundamentally different from NHS stool testing.
In the NHS, we test to answer:
“Is there a disease?”
In functional medicine, we ask:
“Why are symptoms happening in the first place?”
This is where microbiome testing becomes relevant.
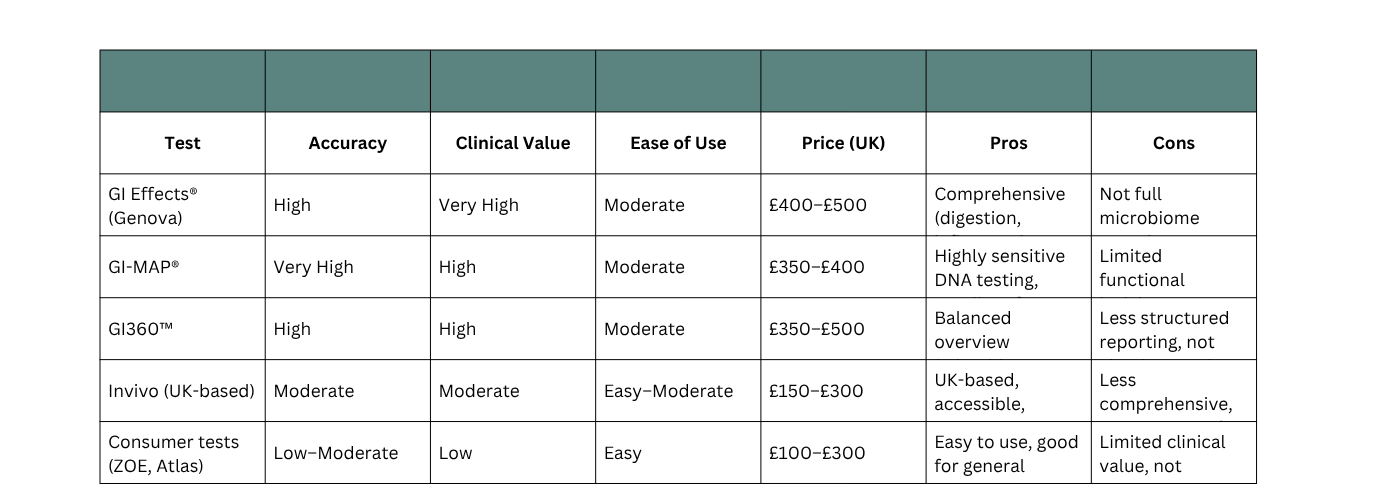
A Closer Look at the Leading Gut Tests in the UK
What they really offer—and what actually matters
When people search for “the best gut test”, they’re usually comparing brands.
But from a clinical perspective, that’s not how we approach it.
Because the value of a test is not in the name—it’s in what it tells us and what we can do with it
As clinicians, we assess gut tests based on three key principles:
1. Accuracy
How reliable is the data?
Can we trust that what we’re seeing reflects what’s actually happening in the gut?
2. Clinical relevance
Does this result help explain the patient’s symptoms? Or is it interesting—but not useful?
3. Actionability
Can we use this information to guide a clear, personalised treatment plan?
This is the key shift: Most tests provide data. Very few provide clinically meaningful direction.
So rather than asking: “Which test is best?”
We ask:
“Which test is most appropriate for this patient, at this stage?”
In the next section, we break down the most commonly used gut tests in the UK, including what they measure, how accurate they are, and when they are actually worth doing.
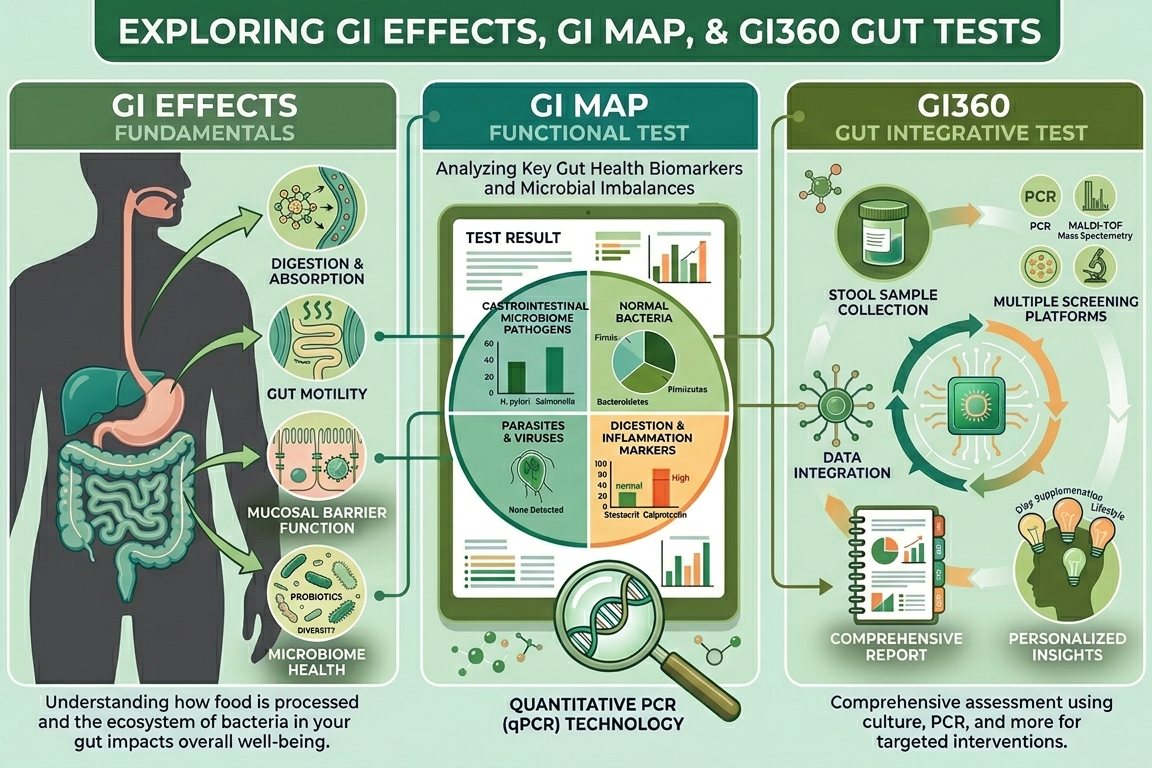
1. GI Effects® (Genova Diagnostics)
A comprehensive, clinically focused gut function test
One of the most commonly used tests in functional medicine—and often our first-line investigation—is the GI Effects® Comprehensive Stool Profile.
Unlike many microbiome tests that focus purely on bacteria, GI Effects provides a broad, functional overview of the gut.
What it measures:
Digestion & absorption (e.g. pancreatic enzymes, fat breakdown)
Inflammation (including calprotectin to help distinguish IBS vs IBD patterns)
Gut immune function (secretory IgA)
Microbiome balance (key bacterial groups)
Pathogens & parasites (via PCR and microscopy)
Accuracy:
GI Effects uses a combination of DNA (PCR), culture, and microscopy, which gives a balanced and clinically useful picture. Strong for:
Detecting inflammation
Identifying digestive dysfunction
Picking up clinically relevant infections
Limitations:
Does not map the full microbiome (targets key organisms only, around 28)
Some bacteria are difficult to detect due to their anaerobic nature
Results need expert interpretation to avoid over- or under-treatment
Clinical value:
This is where GI Effects stands out. It helps answer:
“What is functionally going wrong in this gut?”
Rather than just listing bacteria, it helps us understand:
Is this a digestion issue?
An inflammatory pattern?
Dysbiosis or infection?
Our clinical perspective
GI Effects is often the best starting point when patients present with:
Bloating, IBS, or mixed digestive symptoms
Ongoing symptoms despite “normal” NHS tests
Complex, multi-system health issues
It gives us a clear functional overview, allowing us to prioritise treatment effectively.
2. GI-MAP® (Diagnostic Solutions)
A precision DNA-based microbiome and pathogen test
GI-MAP® is one of the most advanced DNA-based stool tests available and is widely used in functional and integrative medicine when a more targeted, microbiological analysis is needed.
Unlike broader functional tests, GI-MAP focuses on detecting specific microbes with high sensitivity.
What it measures:
Pathogenic bacteria (including H. pylori)
Parasites
Viruses
Fungi/yeast
Commensal bacteria (key groups)
Virulence factors (how aggressive certain microbes are)
Antibiotic resistance genes
Accuracy:
GI-MAP uses qPCR (quantitative DNA technology), which is highly sensitive and specific. Strong for:
Detecting low levels of pathogens
Identifying clinically relevant infections
Providing precise microbial data
Limitations:
Can detect DNA from non-active or dead organisms
Less insight into digestion and overall gut function
Requires careful interpretation to avoid over-treatment
Clinical value:
GI-MAP is best used when we need to answer:
“Is there a specific pathogen or microbial driver we need to target?”
It is particularly useful for:
Suspected H. pylori
Chronic or unexplained gut symptoms
Treatment-resistant cases
Investigating possible parasites or infections
Our clinical perspective
GI-MAP is not usually a first-line test—it is a targeted tool.
We typically use it when:
We suspect a specific infection or microbial imbalance
Or when initial testing suggests something deeper needs exploring
It allows for precision treatment, rather than broad or trial-and-error approaches.
3. GI360™ (Doctor’s Data)
A hybrid test combining microbiome analysis with gut function
GI360™ is another comprehensive stool test that sits between broad functional testing and microbiome analysis.
It combines DNA technology with traditional culture methods, aiming to provide both microbial insight and functional assessment.
What it measures:
Microbiome balance (via PCR and culture)
Pathogens and parasites
Digestion markers (e.g. elastase)
Inflammation markers
Metabolites (including short-chain fatty acids)
Accuracy:
GI360 uses a combination of PCR (DNA) and culture techniques, similar to GI Effects. Strong for:
Providing a broad overview of gut health
Identifying both microbial patterns and functional issues
Limitations:
Culture methods may miss organisms that don’t grow well outside the gut
Microbiome detail is less comprehensive than advanced sequencing tests
Some findings may be less clinically actionable without context
Clinical value:
GI360 helps answer:
“What patterns are emerging across the gut ecosystem?”
It is useful for:
Patients with general digestive complaints
Exploring both function and microbiome together
Situations where a balanced, all-in-one overview is needed
Our clinical perspective
GI360 is a solid, well-rounded test, but in practice:
We tend to favour GI Effects for its clearer clinical framework and actionability.
GI360 may be considered when:
A combined microbiome + function overview is desired
Or when specific practitioner preference or availability plays a role
4. Invivo Gut Health Test (UK-Based Laboratory)
A practical, UK-based option with functional insight
Invivo is one of the few UK-based functional testing laboratories, widely used by nutrition and functional medicine practitioners.
It offers stool testing that combines microbiome analysis with key functional markers, with the advantage of being locally processed and easily accessible in the UK.
What it measures:
Microbiome balance (via DNA analysis)
Pathogens and opportunistic bacteria
Yeast and parasites
Selected digestive and inflammatory markers
Accuracy:
Invivo uses DNA-based testing (PCR/sequencing) alongside selected functional markers. Strong for:
Identifying microbial imbalances
Providing a general overview of gut health
Accessibility and turnaround time within the UK
Limitations:
Less comprehensive than tests like GI Effects for digestion and immune markers
Less depth than GI-MAP for detailed pathogen and virulence analysis
Some panels are more screening-level than diagnostic-level
Clinical value:
Invivo helps answer:
“Is there a general imbalance in the gut microbiome?”
It is particularly useful for:
Patients starting their gut health journey
Mild to moderate digestive symptoms
Situations where a UK-based, accessible option is preferred
4. Consumer Gut Tests (ZOE, Atlas Biomed, GetTested)
Accessible—but limited in clinical value
Consumer gut health tests have become increasingly popular in recent years, driven by growing awareness of the microbiome.
Companies such as ZOE, Atlas Biomed, and GetTested offer at-home kits that provide insights into your gut bacteria, often combined with personalised dietary recommendations.
What they measure:
Microbial diversity
Relative abundance of bacterial groups
General patterns within the microbiome
Some also provide:
Diet scores
App-based nutrition guidance
Accuracy:
These tests typically use DNA sequencing technologies, which are effective for identifying broad microbial patterns. Strong for:
General microbiome trends
Population-level insights
Personalised nutrition guidance
Limitations:
Results can vary between companies
No standard definition of a “healthy microbiome”
Limited clinical validation for diagnosing or treating disease
Clinical value:
These tests help answer:
“How does my microbiome compare, and how might I optimise my diet?”
They can be useful for:
Increasing awareness of gut health
Motivating dietary improvements
General lifestyle optimisation
Our clinical perspective
Consumer tests are not wrong—they’re just limited.
They can be a helpful starting point for understanding your gut health.
But in patients with:
Persistent symptoms
Complex health issues
Or unclear diagnoses
They rarely provide enough depth to guide meaningful treatment.
The real risk of gut testing (that nobody talks about)
Done well, gut testing can be incredibly helpful.
Done poorly, it can lead to:
Confusion
Overwhelm
Unnecessary supplements
Or a treatment that misses the real issue
Because data without context is not clarity—it’s noise.
The bottom line
There is no single “best” gut test, only the right test for the right person, at the right time. Gut microbiome testing can be incredibly valuable, but only when interpreted in the context of your symptoms, history, and overall health.
Without that, it often creates more confusion than clarity. The real value lies not in the test itself, but in clinical insight and a clear, personalised plan.
What to do next
At Lantern Clinic, we combine NHS medical training with functional medicine expertise to guide you through this process properly, choosing the right tests (if needed) and turning results into meaningful action.
If you’ve been struggling with ongoing symptoms or want a deeper understanding of your health, book a discovery call, and we’ll help you map out the next step with clarity and confidence.