SIBO Explained: Symptoms, Causes, Testing and Treatment
What is SIBO and could it be behind your symptoms?
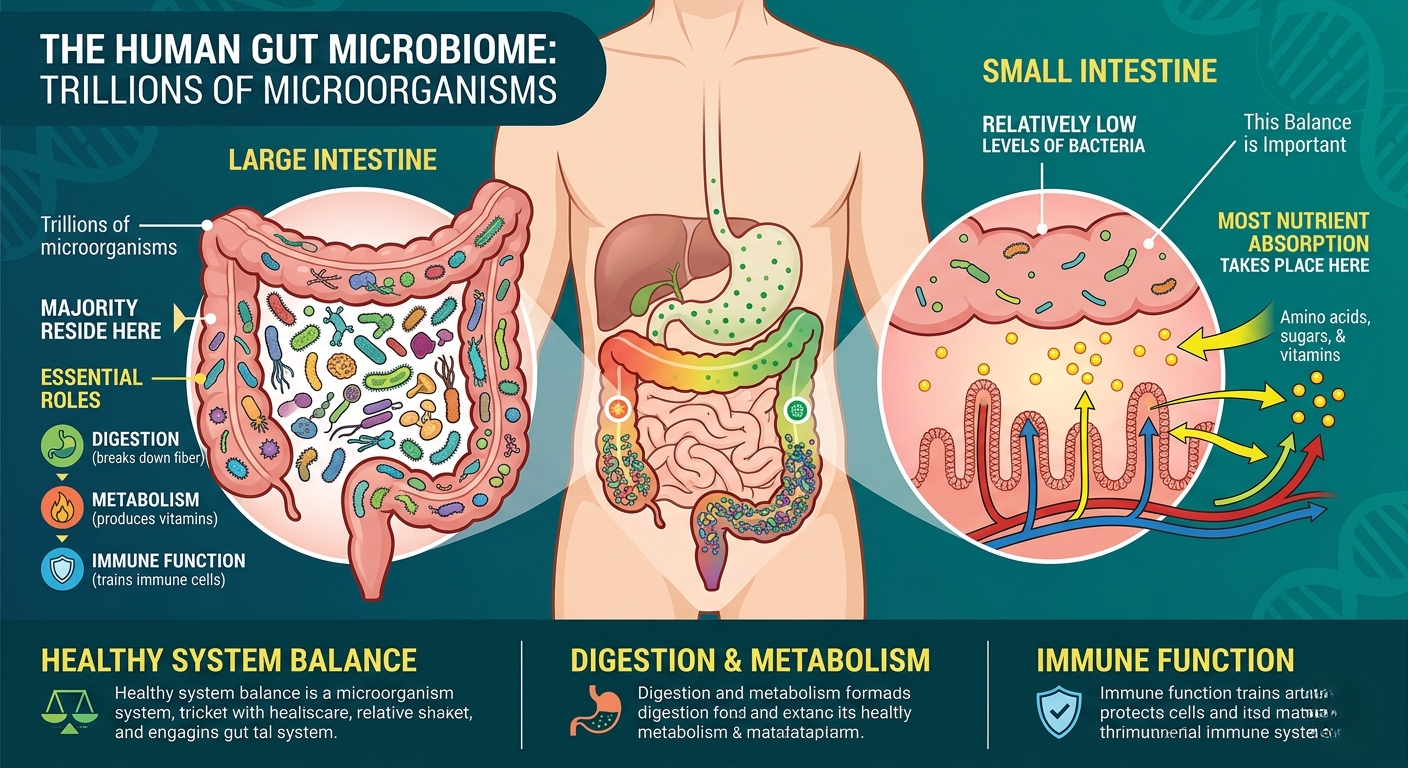
The human gut contains trillions of microorganisms, collectively known as the gut microbiome, which play an essential role in digestion, metabolism, and immune function.
In a healthy system, these bacteria are not evenly distributed. The majority reside in the large intestine, while the small intestine contains relatively low levels of bacteria.
This balance is important, as the small intestine is where most nutrient absorption takes place. SIBO (Small Intestinal Bacterial Overgrowth) occurs when this natural distribution is disrupted, and excessive bacteria begin to accumulate in the small intestine. When this happens, bacteria start fermenting food too early in the digestive process.
This can interfere with normal digestion and absorption, leading to symptoms such as bloating, abdominal discomfort, excessive gas, diarrhoea or constipation. Some individuals also experience fatigue or difficulties with concentration.
SIBO is particularly relevant because of its overlap with irritable bowel syndrome (IBS). Research suggests that a significant proportion of individuals diagnosed with IBS estimates range from around 40% to 70%, may have underlying SIBO contributing to their symptoms.
In the UK, IBS affects approximately 10–20% of the population.
This suggests that a considerable number of people may be living with undiagnosed SIBO, often without access to targeted investigation or treatment. Despite this, SIBO is not routinely assessed within standard clinical pathways. As a result, many patients continue to manage ongoing symptoms without a clear understanding of the underlying cause.
Recognising SIBO as a potential contributor is an important step towards more targeted investigation and effective management.
How Do You Test for SIBO?
Diagnosing SIBO requires a combination of clinical assessment and appropriate testing. As symptoms can overlap with other gastrointestinal conditions, testing helps to clarify whether bacterial overgrowth is likely to be contributing.
The most commonly used investigation is a breath test. This involves drinking a sugar solution (usually lactulose or glucose) and measuring the levels of hydrogen and methane gases in the breath over a period of time. These gases are produced by bacteria, and elevated levels may indicate overgrowth in the small intestine.
Breath testing is non-invasive and widely used in both clinical and functional medicine settings. However, results need to be interpreted carefully, as they can be influenced by preparation, timing, and individual variation.
In addition to breath testing, a comprehensive clinical assessment is essential. This includes a detailed review of symptoms, medical history, diet, medications, and factors that may affect gut motility or microbiome balance.
In some cases, gut microbiome testing may also be used to provide a broader view of bacterial balance in the digestive system. While this does not diagnose SIBO directly, it can offer useful insights into underlying patterns that may contribute to symptoms.
At present, SIBO testing is not routinely available through standard NHS pathways, which means many patients may need to explore private or specialist options if SIBO is suspected.
A structured approach, combining clinical expertise with targeted testing, offers the most reliable way to determine whether SIBO is present and to guide appropriate management.
What Causes SIBO?
SIBO does not usually occur in isolation. In most cases, it develops as a result of underlying imbalances that affect the gut environment and normal digestive function.
One of the key contributors is chronic dysbiosis, an imbalance in the gut microbiome. Over time, this disruption can allow bacteria to expand beyond their usual location in the large intestine and into the small intestine.
Impaired upper digestive function also plays an important role. Adequate stomach acid is essential for controlling bacterial levels as food enters the digestive tract. Reduced acidity, whether due to stress, ageing, or medication, can allow bacteria to survive and proliferate more easily.
The use of proton pump inhibitors (PPIs) and other acid-suppressing medications has been associated with an increased risk of SIBO. By lowering stomach acid, these treatments can alter the natural defence mechanisms that help regulate bacterial growth.
Antibiotic use is another recognised factor. While often necessary, antibiotics can disrupt the balance of the gut microbiome, sometimes leading to longer-term changes in bacterial composition and function.
Chronic alcohol consumption may also contribute. Studies have shown a higher prevalence of SIBO in individuals with alcohol-related liver disease, likely due to combined effects on gut motility, microbiome balance, and intestinal barrier function.
More broadly, SIBO can be understood as part of a continuum of gut dysfunction. Rather than a single isolated condition, it often reflects a progression from dysbiosis and impaired gut regulation.
Are There Different Types of SIBO?
SIBO is not a single, uniform condition. It can present in different ways depending on the types of microorganisms involved and the gases they produce. This variation often explains why symptoms differ from person to person.
The most commonly recognised forms include:
Hydrogen-dominant SIBO
This is the most typical form and is often associated with:
Bloating
Loose stools or diarrhoea
Abdominal discomfort
Hydrogen-producing bacteria ferment carbohydrates in the small intestine, leading to more rapid gas production and digestive upset.
Methane-dominant SIBO (often referred to as intestinal methanogen overgrowth)
This type is linked to a different group of microorganisms called methanogens. It is more commonly associated with:
Constipation
Slower gut motility
A feeling of incomplete bowel emptying
Methane gas appears to slow intestinal transit, which can make symptoms more persistent.
Mixed gas patterns. Some individuals produce both hydrogen and methane gases. In these cases, symptoms may alternate, for example, periods of diarrhoea followed by constipation making the clinical picture less predictable.
What About SIFO?
In some cases, symptoms similar to SIBO may be related to SIFO (Small Intestinal Fungal Overgrowth), where there is an overgrowth of yeast—most commonly Candida species—within the small intestine.
SIFO is less clearly defined than SIBO and can be more difficult to diagnose in routine practice. However, it is increasingly recognised as part of a broader pattern of chronic dysbiosis, where the balance between bacteria and fungi in the gut is disrupted.
This imbalance may develop over time and is often influenced by factors such as:
Repeated or prolonged antibiotic use
Diets high in refined carbohydrates and sugars
Impaired immune or gut barrier function
A high carbohydrate intake can promote fermentation and may support both bacterial and fungal overgrowth. In some individuals, this is associated with increased methane production, slower gut motility, and symptoms such as constipation.
SIFO may be considered when:
Digestive symptoms persist despite treatment for SIBO
There is ongoing bloating, gas, and gut sensitivity
There are additional features suggestive of fungal involvement
These can include:
Recurrent oral thrush
Frequent fungal skin infections
Persistent sugar cravings
In clinical practice, mixed patterns are not uncommon. Some individuals may have overlapping bacterial and fungal overgrowth alongside wider microbiome disruption.
Recognising this broader context is important, as it helps guide a more individualised and comprehensive approach rather than focusing on a single diagnosis in isolation.
What to Do Next If You Suspect SIBO
If several of the symptoms and patterns described feel familiar, it may be worth exploring SIBO further as a possible contributor.
The first step is a careful clinical assessment. Many digestive symptoms overlap with other conditions, so it is important to take a structured history and consider the wider context—diet, medications, stress, and overall health.
Where appropriate, breath testing can be used to assess for bacterial overgrowth. This is a non-invasive test that provides useful information when interpreted alongside clinical findings.
In some cases, broader functional testing of the gut microbiome may also be helpful. While this does not diagnose SIBO directly, it can offer insight into underlying dysbiosis and guide a more personalised approach.
It is also important to recognise that managing SIBO is rarely about a single intervention. A comprehensive approach may include:
Supporting digestive function
Addressing diet in a structured and sustainable way
Considering targeted antimicrobial or medical treatment where appropriate
Improving gut motility and overall gut environment
Equally important is ongoing follow-up, as symptoms and responses to treatment can evolve. If symptoms have been persistent or if previous approaches have not led to lasting improvement, a more structured and individualised assessment may be beneficial.
Can SIBO Be Treated and Does It Come Back?
SIBO can be treated, and many people experience significant improvement in their symptoms with the right approach.
Treatment typically focuses on reducing bacterial overgrowth and improving the function of the digestive system. This may involve dietary strategies, targeted antimicrobial treatment (medical or herbal), and support for gut motility.
However, an important consideration is that SIBO has a tendency to recur, which is very common and problematic. This is because, in many cases, SIBO is not the primary problem but rather a consequence of underlying factors such as impaired gut motility, chronic dysbiosis, or reduced stomach acid. If these contributing factors are not addressed, symptoms may return over time.
For this reason, a more effective approach often involves:
Identifying and addressing underlying drivers
Supporting normal digestive function
Gradually restoring a balanced gut environment
Recovery is often a process rather than a single intervention, and timelines can vary depending on the individual and the complexity of their symptoms. With a structured and personalised approach, many people are able to achieve meaningful and sustained improvement.
How Is SIBO Treated?
SIBO treatment involves more than simply reducing bacterial overgrowth. A structured approach is usually required, combining targeted antimicrobial therapy (either antibiotics or carefully selected herbal protocols) with support for digestion, gut motility, and the wider microbiome. At Lantern Clinic, we follow a functional framework similar to the 5R approach: removing excess bacteria, supporting digestive function, rebalancing the microbiome where appropriate, and addressing underlying drivers such as low stomach acid or impaired motility.
Diet also plays an important role, particularly in reducing symptoms during treatment. A temporary reduction in fermentable carbohydrates may help, but overly restrictive diets are not a long-term solution and should be carefully managed. Importantly, SIBO shares symptoms with other gastrointestinal conditions, including coeliac disease and inflammatory bowel disease, so a doctor-led approach is essential to ensure accurate diagnosis and safe, effective treatment.
Self-treatment, particularly with antimicrobials, can lead to incomplete resolution or recurrence if the underlying causes are not addressed.
Final Thoughts
SIBO is a common but often overlooked cause of persistent digestive symptoms. While it shares features with conditions such as IBS, it represents a more specific disruption in the balance and function of the gut microbiome—one that requires a structured and individualised approach.
If you have ongoing symptoms that have not responded to standard treatments, it may be worth considering whether SIBO is contributing. A careful clinical assessment, supported by appropriate testing, can help clarify the picture and guide a more targeted and effective plan for recovery.